
Sometimes called “Benzos”, Benzodiazepines are a class of drugs with sedative and hypnotic effects that depress the central nervous system (CNS) 2. They have a calming (sedative) effect and are often prescribed to relieve acute anxiety. Because they also have a hypnotic effect, they can also be prescribed to treat sleep problems. Benzodiazepines are sometimes used during alcohol detoxification because they have an anticonvulsant effect.
TL;DR: Benzodiazepine addiction can develop quickly, worsen mental health over time, and pose serious risks during withdrawal—but with expert, evidence-based care like Tree House Recovery’s California rehab programs, full recovery is possible.
Benzos are prescribed to manage various medical and mental health conditions. While they are considered generally safe and effective when used as directed, they have a strong potential for misuse, like all Schedule IV controlled substances.
Here’s what benzos are used for:
Benzos can be helpful in all these cases, but their use is almost always limited to avoid the risk of misuse and dependence.
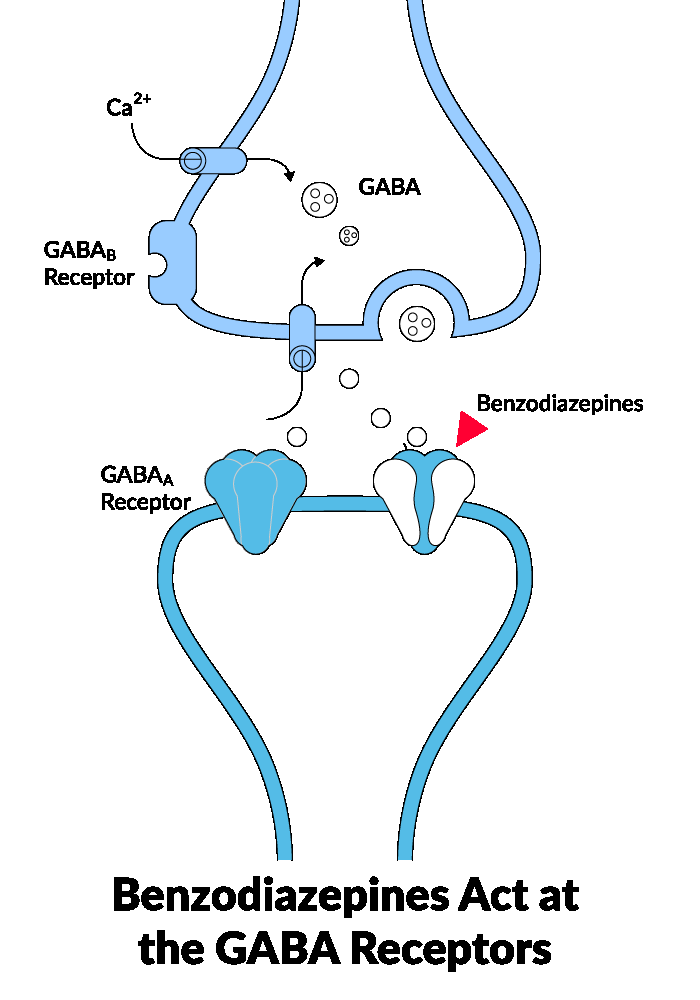
“How do benzos work” is a common question asked by those prescribed this class of medication. The drugs affect neurotransmitters in the brain—chemical messengers that help regulate mood, behavior, and physical responses. Benzos specifically target GABA (gamma-aminobutyric acid), the brain’s primary calming neurotransmitter.
GAB naturally slows activity in the CNS (central nervous system), reducing anxiety and encouraging the body to relax. When benzodiazepines are introduced, they bind to GABA-A receptors in the brain, enhancing the effects of GABA. This results in the following:
The same mechanism that helps relieve anxiety can lead to the development of dependence, though. This means the brain starts to rely on benzos for calmness, making it difficult for a person to feel normal without them. For this reason, benzos are typically prescribed only for short-term use.


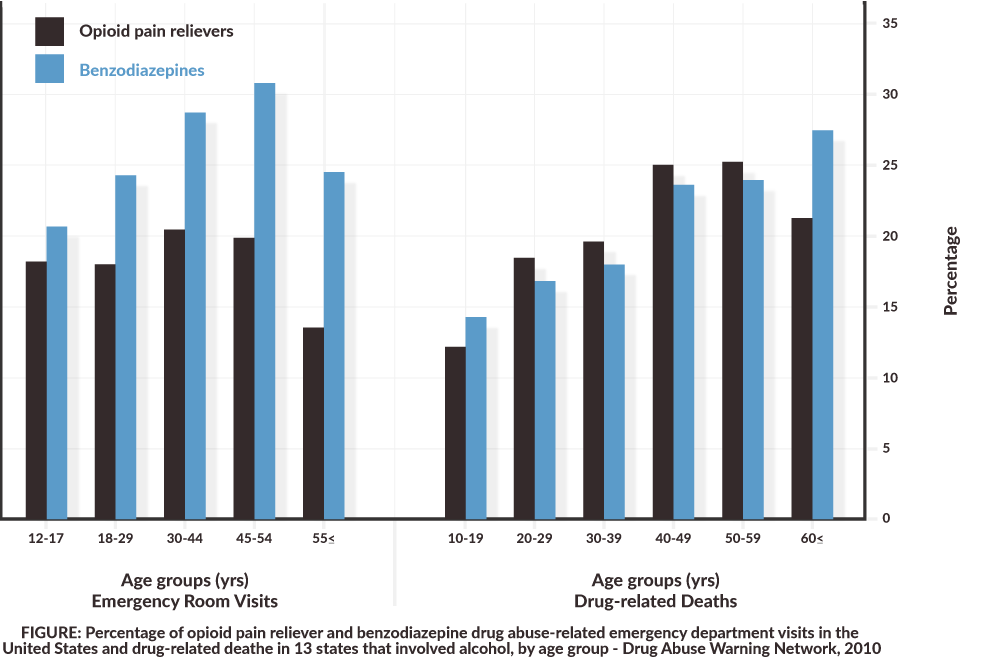

List of short and long-term physical effects of Benzodiazepine Abuse: 10, 11, 12
Short and long-term mental effects of benzodiazepine abuse:10, 11, 12
Like all addictive drugs, benzodiazepines increase the amount of dopamine (a neurotransmitter that creates happiness). Individuals who are vulnerable to crave the surge of euphoria caused by the drug quickly begin abusing it to recreate this feeling as much as possible.
But people become dependent on benzodiazepines, even if they are not trying to abuse them. Physical dependence on these drugs forms very quickly, meaning that if a person stops taking the drug, they will feel withdrawal symptoms that often begin with a magnified version of the symptoms that prompted them to use in the first place.8
To avoid the pain of withdrawal, people will begin drug-seeking behaviors if they run out (e.g, lying to doctors, family, or friends to get pills, buying pills online or from dealers, stealing pills or money).12
Discontinuing the use of benzodiazepines can be challenging, especially if you’ve taken them for an extended period or at high doses. A safe and streamlined withdrawal process involves careful planning, medical oversight, and ongoing support.
1) Recognizing the need for change
Acknowledging the risk of benzodiazepine dependence is the first fundamental step. Whether you’re misusing benzos or taking them as prescribed, deciding to quit can feel overwhelming at first. However, taking that first step is a powerful and empowering way to start your recovery journey.
Benzodiazepine withdrawal can be life-threatening if not managed properly. Seizures, severe anxiety, and hallucinations are some risks of stopping benzos abruptly. A medically supervised detox ensures safety throughout the tapering process. Here’s what happens during detox:
After detox, entering a rehab program can provide the structure and tools you need for long-term recovery from benzo dependence.
Inpatient programs provide 24/7 care in a highly structured environment with therapy, holistic treatments, and support groups. This works best for those with severe addictions or co-occurring mental health disorders. Outpatient programs enable individuals to receive treatment while living at home and meeting their everyday obligations, ideal for those with milder addictions and stable home environments.
Recovery doesn’t end after detox or rehab. A comprehensive aftercare plan helps people stay sober long-term. This may include:
5) Building a robust support network
Recovery is a journey best taken with the help of others. Rely on friends, family, and recovery professionals to guide and encourage you.
Do not attempt to quit benzodiazepines cold turkey without medical guidance—the risks are too high, and the process is far more effective with clinical assistance.
At Tree House Recovery, we are proud of the program we’ve built to create sustainable sobriety. Our method works. We use eight connected treatments to help our patients understand the cause of their addiction, the pathology of the disease, how to cope, deal with stress, and reset their brain chemistry. Our graduates become someone they’ve never met before — a person who’s deeply confident, strong, at peace with themselves, and most importantly, happy.
For more information: See reviews from former patients, our success rates, read about our staff, or take a look at our facilities.
Disclaimer:
No content on this website should ever be used as a substitution for direct medical care and advice from a qualified physician clinician.
Benzodiazepines are prescription drugs that slow brain activity. They are used to treat anxiety, panic attacks, muscle spasms, and insomnia. They work by increasing calming chemicals in the brain.
Common benzos include Xanax, Valium, Klonopin, and Ativan. These drugs are often prescribed for short-term use but can quickly lead to dependence.
Yes, benzos are highly addictive. Dependence can form in just a few weeks. Withdrawal can be dangerous without medical help.
Benzos are central nervous system depressants. They are classified as Schedule IV controlled substances because of their abuse potential.
Most insurance plans do cover benzo addiction treatment. At Tree House Recovery, we work with many major providers. Our team helps you verify coverage and plan your care.
