TRICARE insurance provides coverage for active-duty service members, National Guard and Reserve members, retirees, their families, survivors, and certain former spouses worldwide. It offers comprehensive health coverage, including medical, dental, and prescription coverage. TRICARE is managed by the Defense Health Agency (DHA) and operates similarly to a traditional health insurance plan, but with specific benefits tailored to the unique needs of military members and their families.
Does TRICARE cover addiction Treatment? Yes, TIRCARE does cover emergency and non-emergency inpatient hospital care for substance abuse disorders. Inpatient services are made available for you if you need to stabilize, detox, or have any complications from your addiction.
You have coverage for inpatient hospitalization for substance use disorders and other mental health through TRICARE. Inpatient care is there for you when you need around the clock care with medically monitored treatment.
You may get TRICARE approval for inpatient care if you are at risk of harming yourself or others due to your substance abuse. If an outpatient level of care is not adequate for your treatment needs, it would be appropriate to begin inpatient care.
If you have a substance use disorder or SUD, TRICARE covers emergency inpatient hospital services for:
If your addiction stops you from normal functioning, you can’t function at an outpatient level of care and need 24-hour supervision, TRICARE may approve your residential care. Residential treatment can sometimes be part of the treatment plan. It sometimes is the second step right after you go through detox and may depend on the extent of use and level of structure and supervision deemed necessary. You are not expected to know the level of care you need. We can guide you through the confidential assessment so you can get the help you need.
Tree House Recovery has helped many people with TRICARE insurance. Our holistic program is an approach that offers more than talk-therapy. We focus on sustainable health outcomes that rebuild your mind, body and spirit so you get healthy and stay sober. Our goal is to ensure your experience in rehab is the first, only or last time needed.
Optimize your life:
Some TRICARE plans, such as TRICARE Reserve Select, TRICARE Young Adult, and TRICARE Prime Remote, can opt to receive treatment from an out-of-network provider, but the costs are higher than using an in-network provider. Other plans require you use an in-network provider. An in-network provider with TRICARE can offer you the least expensive coverage as the rates negotiated between a provider and the insurance plan are usually the best possible value. Also keep in mind that some providers will require payment up front for the entire cost of treatment and you may have to wait several weeks for TRICARE to reimburse you. This cost could range anywhere from hundreds of dollars for outpatient treatment to thousands of dollars for inpatient treatment.
Beneficiaries can always choose TRICARE network providers. However, you may prefer to go to a center that is out-of-network. Fortunately, with TRICARE, you may find the provider that you want in their list non-network providers. You may receive higher out-of-pocket costs with a non-network provider, but that may not always be the case. Every situation is different. To find out what your policy covers at Tree House, call us anytime.
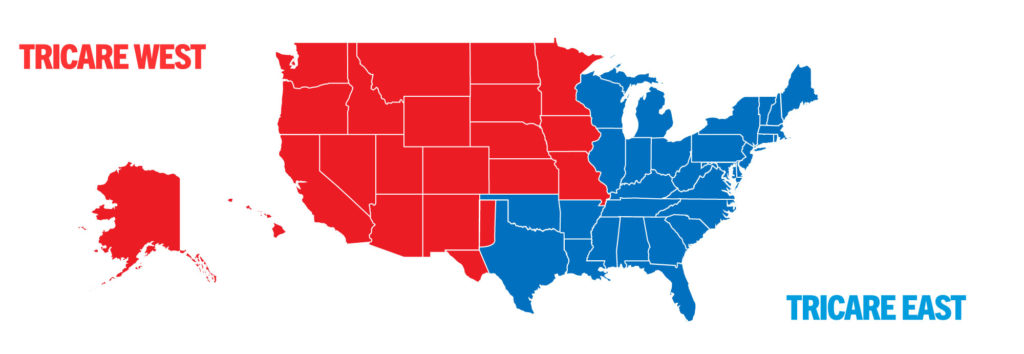
Choosing between TRICARE East and TRICARE West can be a pivotal decision for military personnel and their families. TRICARE East covers a vast region extending from the Eastern Seaboard to the Midwest, while TRICARE West serves the Western United States, including Alaska and Hawaii. The choice depends on factors like your current location, healthcare needs, and available providers.
You have options if you want to find a recovery center that works with TRICARE. First, you can call the center of your choice directly. Ask them if they can check your benefits. They should be happy to help you by verifying your benefits. Or, you can visit a TRICARE website and search for coverage in-network, and non-network providers through their provider portal. Realizing that you need help and reaching out is a huge step in recovery, and we understand that it finding the right treatment center can feel overwhelming. Just know that you have TRICARE and many rehabs that are here to help you navigate your next steps. Call us, and we will help you.
For TRICARE approved residential treatment centers, detoxes, partial hospitalization rehabs, and other options see the links below:
TRICARE Prime: Managed care option offering the most affordable coverage. Available in stateside Prime Service Areas and overseas.
TRICARE Select: Self-managed care option offering the most freedom of choice. Available to most beneficiaries worldwide except active duty service members and certain others.
US Family Health Plan: A TRICARE Prime plan offered by not-for-profit health care systems in six areas of the United States.
TRICARE Reserve Select: A health plan available for purchase by qualified members of the Selected Reserve, their family members, and qualified survivors.
TRICARE Retired Reserve: A health plan available for purchase by qualified members of the Retired Reserve, their family members, and qualified survivors.
TRICARE Young Adult: A health plan that qualified adult children of eligible sponsors may purchase.
TRICARE For Life: Medicare wraparound coverage that begins automatically once you have Medicare Part A and Part B. Overseas, where Medicare doesn’t provide coverage, TFL is the primary payer.